Difference Between ocular hypertension and glaucoma
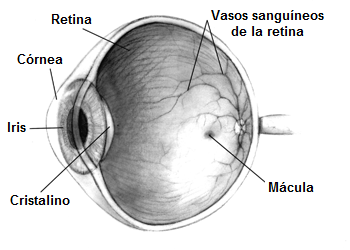 Ocular hypertension vs glaucoma
Ocular hypertension vs glaucoma
The structures within the eye maintain its spherical shape. To do this, they exert a certain amount of outward pressure called intraocular pressure. The normal range of this intraocular pressure is between 10 to 21mmHg. Elevation in this pressure for any reason is termed as Ocular hypertension. It is an elevated pressure within the eyeball without loss of vision, reduction in visual field or optic nerve damage. Glaucoma, in contrast, is a serious medical condition that must be immediately brought to a certified ophthalmologist’s attention and adequately treated. Glaucoma is characterised by progressive damage to the optic nerves leading to loss of vision if left untreated.
Ocular hypertension can affect people in any age group but is more common in people above 40, those having a strong family history of glaucoma or ocular hypertension, diabetics and very near-sighted. Glaucoma, can be present since birth, albeit rare, or acquired later, especially beyond 40. It is the second commonest cause of blindness in the U.S. Conditions like chronic inflammation of eyes, a thin cornea and use of medications that increase intraocular pressure like corticosteroids in oral/topical form, tricyclic anti-depressants, anti-psychotic drugs, anti-spasmodic medications, anti-histamines, etc. Sulpha containing medications may also produce glaucoma and thus must be used with great caution.
Ocular hypertension is a major risk factor for developing glaucoma but glaucoma can develop even when the intraocular pressure is normal. This is termed as normal-tension glaucoma. The reason behind it is unknown but there is definite nerve damage despite normal pressures. Physical injuries to the eye and medical conditions like diabetes and hypertension may lead to glaucoma as well.
The exact cause of glaucoma or ocular hypertension is not known to modern medicine as yet. The two main mechanisms of development of these conditions are either an increased production of the aqueous humour in the eye or a reduced outflow and circulation of aqueous humour.
Ocular hypertension doesn’t produce any signs or symptoms since it does not damage any tissues within the eyes. Thus, it might be persisting for a while before your doctor finds out that you have an elevated pressure by using an instrument called the tonometer. Glaucoma damages the optic nerve cells and manifests as blurring of vision, reduction in the field of vision and sometimes as an acute attack of blindness. Angle-closure glaucoma is a rare type of glaucoma which presents with sudden blindness, nausea, redness of the eye, coloured rings around lights in the field of vision and pain in the eye. It is precipitated by a sudden rise in the intraocular pressure closing the angle through which the fluids of the eye circulate and maintain pressure.
Diagnosis is made by using a tonometer to check intraocular pressure and pachymetry to assess corneal thickness. Perimetry is done to gauge visual field loss.
Treatment is available for both ocular hypertension and glaucoma. Pilocarpine, timolol, clonidine and acetazolamide are used commonly as eye drops to treat ocular hypertension. Glaucoma can be treated with eye drops, laser or conventional surgery and drainage implants.
TAKE HOME POINTERS:
Ocular hypertension is an elevated pressure within the eye without damage to any optic structures, without visual field loss or blindness.
Glaucoma is a serious medical condition of elevated intraocular pressure with optic nerve damage and blurred vision/blindness/pain in eye.
Ocular hypertension is a risk factor for glaucoma but glaucoma can occur in those with a normal intraocular pressure too.
The exact cause for either are not known but can be precipitated by certain medications.
Both are treatable. Glaucoma requires immediate treatment and may lead to permanent blindness if left untreated.
- Difference Between Vascular Cambium and Cork Cambium - November 1, 2023
- Difference Between DevOps and Developer - September 10, 2023
- Difference Between Acute Gastritis and Chronic Gastritis - April 3, 2023
Search DifferenceBetween.net :
Leave a Response
References :
[0]http://emedicine.medscape.com/article/1205298-overview
[1]http://www.mayoclinic.com/health/glaucoma/DS00283/DSECTION=causes
[2]http://en.wikipedia.org/wiki/Glaucoma
[3]http://en.wikipedia.org/wiki/Ocular_hypertension
[4]http://www.aoa.org/patients-and-public/eye-and-vision-problems/glossary-of-eye-and-vision-conditions/ocular-hypertension
[5]http://www.aoa.org/patients-and-public/eye-and-vision-problems/glossary-of-eye-and-vision-conditions/glaucoma
